As a parent of a child with cerebral palsy, you may have heard the term spasticity before. Spasticity is a common condition that affects children with cerebral palsy and can have a significant impact on their daily life. It’s important to understand what spasticity is and how it can be managed to help your child reach their full potential. In this article, we will provide an overview of spasticity in children with cerebral palsy, its causes, common problems associated with spasticity, and available treatments.
TL;DR – the highlights:
- spasticity is a common condition in children with cerebral palsy and is caused by damage to the motor control centers of the brain
- spasticity can cause muscle stiffness and tightness, which makes it difficult for children with cerebral palsy to move and perform everyday activities
- common problems associated with spasticity include contractures, pain, and difficulty with hygiene and care
- treatment options for spasticity include physical therapy, medications, and surgery
- the goal of managing spasticity is to improve function, mobility, and quality of life
What is spasticity?
Spastic cerebral palsy (CP) is the most commonly diagnosed disorder in children with CP.1 It’s a movement disorder characterized by increased muscle tone, stiffness, and involuntary muscle contractions. Simply put, this means that the muscles are constantly contracted or tight, which can cause problems with movement and coordination. It can affect the whole body, but is generally worse in the lower limbs of children with bilateral involvement and in the upper limbs of children with unilateral involvement.2
In children with CP, spasticity is often caused by damage to the developing brain that controls movement, which can occur before birth, during birth, or in the first few years of life. Damage to the brain’s motor control centers disrupts normal communication between the brain and muscles, leading to increased muscle tone and stiffness. This makes it difficult for children with CP to move and perform daily activities, such as sitting, standing, walking, and grasping objects.
NOTE: It’s important to know that spasticity is not caused by muscle weakness, but rather by the way the brain communicates with the muscles.
Influence of spasticity
Spasticity can significantly affect a child’s daily life, including their mobility, ability to perform activities of daily living, and overall quality of life. Some common problems associated with spasticity include:
1. Contractures
Long-term spasticity combined with muscle weakness and soft tissue changes, as seen in spastic CP, can cause muscles to shorten and become tight, resulting in contractures or permanent shortening of the muscle-tendon unit. Contractures can limit a child’s range of motion and make it difficult to perform daily activities and can also cause pain and discomfort.
2. Pain
Spasticity can cause muscle pain and discomfort, which can affect a child’s ability to participate in physical activities and social interactions. Pain is common in spastic CP, with a reported prevalence of 65−78%. Most pain complaints in children with spastic CP are in the form of secondary conditions, often caused by joint deformities and misalignment, muscle spasms, and contractures. The pain itself can also cause muscle spasms at the affected point. Other causes of muscle spasms are fatigue, inflammation, and overuse.3
3. Difficulty with activities of daily living (ADLs)
Spasticity can make everyday tasks such as dressing, bathing, and eating difficult for children. Spasticity can make it difficult for children with CP to maintain good hygiene and care. This can lead to frustration and loss of independence.
4. Feeding problems
The presence of motor dysfunction in spastic CP affects their ability to feed, probable causes include inadequate postural control, involuntary movements, immobility, inability to self-feed, and difficulty seating. A stable posture is necessary to achieve functional and safe feeding. Limited oromotor function in CP increases susceptibility to aspiration due to abnormal head posture.4
5. Mobility problems
Spasticity can affect a child’s ability to move, walk, and balance. This can make it difficult to move around, participate in sports or other physical activities, and access different environments. Spasticity is thought to interfere with voluntary control and increase energy expenditure during movement.5 Additionally, it interferes with normal muscle lengthening during growth and is thought to contribute to the development of secondary muscle and soft tissue contractures and to skeletal deformation.6
6. Hip subluxation
Hip subluxation is a common progressive condition found in CP children and is attributed to spasticity and contracture of the hip adductors and flexors as well as the medial hamstrings, which leads to dislocation if untreated. These muscles pull the proximal femur into adduction, flexion, and internal rotation, constructively guiding the femoral head away from the hip joint resulting in subluxation. Another factor that can cause subluxation is abductor muscle weakness.7,8
7. Scoliosis
Scoliosis in CP is the combined result of spasticity, muscle imbalances around the spine, and poor muscle control that contribute to impaired trunk control.9 It’s still unknown whether this is directly related to the primary brain injury or to secondary impairments, such as muscle weakness, spasticity, poor balance, or non-ambulatory status.10
Treatment options for spasticity
The goal of treating spasticity is to improve the child’s function, mobility, and quality of life. Spasticity can be treated in different ways, depending on the severity of the condition and the goals of the therapy. Treatment options include physical therapy, orthotics, medications, and surgery.
Physical therapy
Physical therapy is often the first-line of treatment for spasticity in children with CP. A physical therapist can help improve a child’s range of motion, strength, and coordination, which involves a range of exercises and techniques. This can help reduce spasticity and prevent contractures. Physical therapy can also help improve posture and balance, which can improve mobility and prevent falls. In addition, physical therapists may use modalities such as stretching, heat or cold therapy, and massage to help reduce spasticity and improve muscle function.
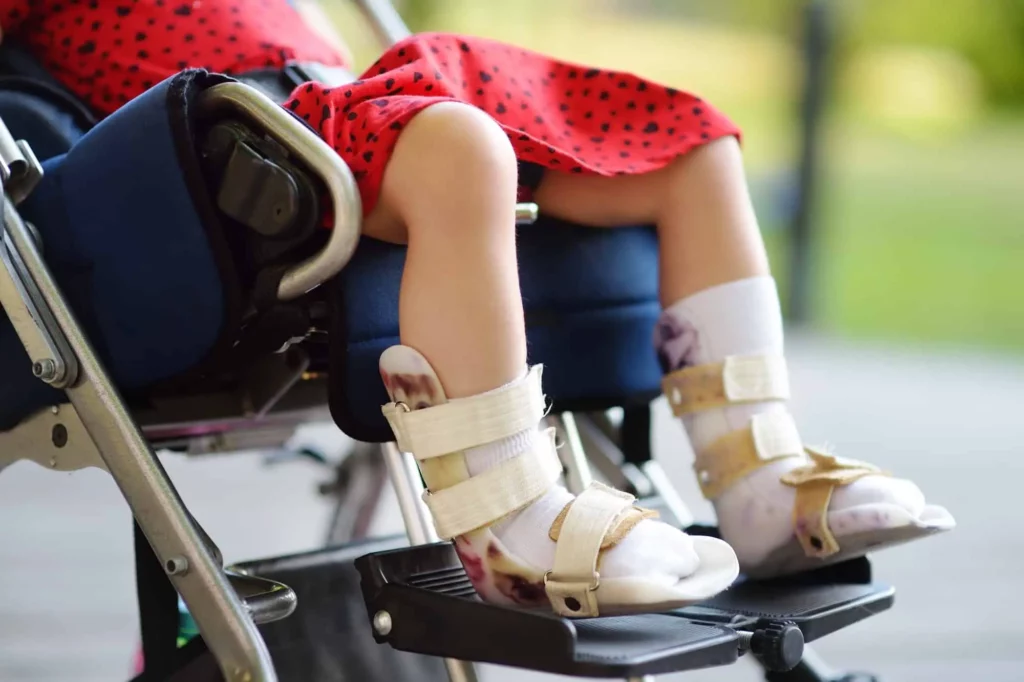
Physical therapists can also help children with spasticity find adaptive equipment, such as standers and orthotics. Orthotics, such as braces or splints, can be used to improve joint alignment and prevent contractures in a spastic limb and/or to help children with CP overcome activity limitations, such as problems with standing and walking.
Medications
There are several medications that can be used to manage spasticity in children with CP, such as muscle relaxants, anti-spasticity medications and botulinum toxin injections. They can help reduce spasticity, improve the child’s mobility and functioning.
Muscle relaxants, such as baclofen, work by reducing the activity of the nerves that control muscle contractions. Anti-spasticity medications, such as tizanidine, work by reducing the excitability of the nerves that control muscle contractions. These medications work by reducing muscle tone and spasticity, but they can also have side effects such as drowsiness and weakness.
Botulinum toxin injections can be used to temporarily reduce spasticity in certain muscles. The toxin works by blocking the release of a chemical messenger that causes muscles to contract. The effects of the injection usually last for several months, after which the injection may need to be repeated. Botulinum toxin can be injected directly into the affected muscles to temporarily paralyze them and reduce spasticity. This treatment is often used for focal spasticity that affects only one or a few muscles. Injecting botulinum toxin can help improve a child’s ability to walk or use their hands and allow the orthotic to fit better by reducing spasticity.
Surgery
Surgery is usually considered a last resort when other treatments have not been effective. This may involve lengthening the affected muscles to improve the child’s function and mobility or surgical interventions, such as selective dorsal rhizotomy by cutting the nerve pathways that cause spasticity.
Selective dorsal rhizotomy (SDR) is a neurosurgical operation on the nerves that enter the spinal cord. The aim of SDR is to improve gross motor function, particularly the ability to walk, by reducing muscle spasticity.
Intrathecal baclofen is a surgically implanted system used to control spasticity. This treatment involves the use of a pump that delivers a continuous dose of baclofen directly into the spinal cord. This can help reduce spasticity throughout the body but is generally reserved for severe cases that haven’t responded to other treatments.
In some cases, surgery may be needed to release tight muscles or correct joint deformities. However, orthopedic surgery is not an option to manage spasticity. Instead, it’s used to help correct secondary problems that occur with growth due to spastic muscles and poor movement control. These problems include muscle shortening, joint contractures and bony deformities.
It’s important to note that the management of spasticity is often a multidisciplinary effort involving various health professionals such as physical therapists, occupational therapists, pediatricians, and neurologists.
REFERENCE:
- Cans Cristine. Surveillance of Cerebral Palsy in Europe. Surveillance of cerebral palsy in Europe: a collaboration of cerebral palsy surveys and registers. Surveillance of Cerebral Palsy in Europe (SCPE). Dev Med Child Neurol. 2000 Dec;42(12):816-24. doi: 10.1017/s0012162200001511
- Sakzewski L, Ziviani J, Boyd R. Systematic review and meta-analysis of therapeutic management of upper-limb dysfunction in children with congenital hemiplegia. Pediatrics. 2009 Jun;123(6):e1111-22. doi: 10.1542/peds.2008-3335
- Vinkel MN, Rackauskaite G, Finnerup NB. Classification of pain in children with cerebral palsy. Dev Med Child Neurol. 2022 Apr;64(4):447-452. doi: 10.1111/dmcn.15102
- Wahyuni LK. Multisystem compensations and consequences in spastic quadriplegic cerebral palsy children. Front Neurol. 2023 Jan 9;13:1076316. doi: 10.3389/fneur.2022.1076316
- Sussman MD. J. R. Gage, M. H. Schwartz, S. E. Koop, T. F. Novacheck (eds): The identification and treatment of gait problems in cerebral palsy. J Child Orthop. 2010 Apr;4(2):177–8. doi: 10.1007/s11832-010-0244-z
- Morrell DS, Pearson JM, Sauser DD. Progressive bone and joint abnormalities of the spine and lower extremities in cerebral palsy. Radiographics. 2002; 22(2):257–268.
- Yildiz C, Demirkale I. Hip problems in cerebral palsy: screening, diagnosis and treatment. Curr Opin Pediatr. 2014 Feb;26(1):85-92. doi: 10.1097/MOP.0000000000000040
- Aroojis A, Mantri N, Johari AN. Hip Displacement in Cerebral Palsy: The Role of Surveillance. Indian J Orthop. 2020 Jun 11;55(1):5-19. doi: 10.1007/s43465-020-00162-y
- Hägglund G, Pettersson K, Czuba T, Persson-Bunke M, Rodby-Bousquet E. Incidence of scoliosis in cerebral palsy. Acta Orthop. 2018 Aug;89(4):443-447. doi: 10.1080/17453674.2018.1450091
- McCarthy JJ, D’Andrea LP, Betz RR, Clements DH. Scoliosis in the child with cerebral palsy. J Am Acad Orthop Surg. 2006 Jun;14(6):367-75. doi: 10.5435/00124635-200606000-00006




